Another comment from CMAS. I think it was Alison Richardson who was presenting at one point and remarked, “but of course we can’t tell where the foot is from the graphs”. How true? and why not? Conventionally in clinical gait analysis we plot where the pelvis is in relation to the lab, then the hip, knee and ankle joints. In theory if you know all this information you can work out the orientation of the foot. I don’t know anyone, however, who has developed the knack of adding all those angles up in their head to work this out. In understanding how the foot is contributing to that pattern I think Perry’s concept of foot rockers is key – is the limb pivoting primarily around the heel, the ankle or the MTP joint? Yet, despite what you hear in many discussions about gait data, it’s virtually impossible to tell from the graphs which rocker is active at any given time.
So why don’t we plot out foot orientation? We calculate the equivalent in the transverse plane and call it foot progression. I think it would make all our lives considerably easier if we added an extra graph at the foot of the sagittal plane data. Given that the pitch of a shoe is how much it tilts the foot forwards perhaps we should refer to this a “foot pitch”.
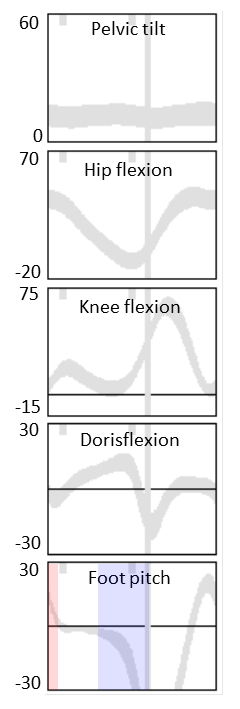
I’ve shown you what the sagittal graphs would then look like. I don’t suggest using the colours on the foot pitch graph – they are only there to show you how easily you can pick out the three rockers. During the red phase of stance the foot is pivoting about the heel – first rocker. During the white phase the foot is flat on the ground – second rocker. During the blue phase the foot is pivoting about the MTP joint (or toe) – third rocker (or third and fourth rockers if you want to use Perry and Burnfield’s most recent terminology (2010). Notice that end of first rocker does not coincide with opposite foot off but is completed appreciably earlier. Many people don’t appreciate just how early third rocker starts either.
.
.
Perry, J., & Burnfield, J. M. (2010). Gait analysis: normal and pathological function (2nd ed.). Pomona, California: Slack.
Well Richard, I think what we should all be looking at is not so much the orientation of the foot relative to vertical or the floor (interesting though this is), and not specifically the joint angles above the foot, but what should REALLY interest us is what is the orientation, relative to vertical, of the shank and thigh segments in mid to late stance. Gait software etc doesn’t tend to give us this info which is a pity, but this is really crucial. What is vital in gait is this. During the period mid to late stance, the thigh needs to incline forward sufficiently and the GRF must pass in front of the knee and behind the hip joint centres to provide passive stability at these joints. In this way the second hump of the GRF is created and deceleration of the CoM is achieved. Many (and probably in my clinical experience most. See Sheila Gibbs’ and my paper in G&P on Ben Lomonding) of our patients cannot achieve this and we must orientate our treatment plans to enable them to do this.
Thanks Barry, I agree with a lot of this. Elaine Owen has popularised a distinction between segment kinematics (alignment of segments with respect to the lab) and joint kinematics (alignment of the distal segment relative to the proximal) and I’d agree that this can really help with some aspects of interpretation. In Melbourne we used some BodyBuilder code (VICON, Oxford) I had written to calculate “projection angles” which where then plotted in our standard Polygon template (VICON again) in the same format as the more usual gait graphs. These showed the projection of the principal axis of the segments onto the relevant laboratory planes. I’ll see if I can get this posted to our download page.
Where I might just question what you’ve written is in the use of the term “passive stability”. I’m sure getting the ground reaction in front of the knee but behind the hip is useful but I’m not convinced that the limb is any more stable in this position than in any other within its joint ranges of movement. From what we know of the anatomy and material properties of the ligaments they act to resist movement at the end of joint range (with the possible exception of the cruciate ligaments). Although the knee is at its most extended in late stance it is generally in some flexion and is thus not at the end of its range of motion (certainly not in the healthy population). The hip is probably closer to end range of extension but I’d still suggest is probably not there yet. I thus doubt if, in normal walking, there is any passive stability associated with this position. Children with cerebral palsy often have joint contractures and the mechanism may operate in them. Perhaps this is a question that a relatively simple research question could answer.
Just want to reiterate that I can quite accept that this alignment is a good thing to attain. Its only the language and the potential mechanism it reflects that I think is worth exploring further.
Well hello boys! Been awhile, hasn’t it? I was just hunkering down for a cyclone here in tropical far north Queensland and found this page. Surely the ‘stability’ afforded by the GRF is not necessarily lock the knee, but to resist its collapse? So any external extensor moment would be helpful in this respect. Look forward to more discussions like this, though I confess I’m a bit out of touch these days!
Hi Chris, great to hear from you again. You have put your finger right on it. I may, or may not, have used the optimum language and am quite happy to change to something better, but what I was trying to say was exactly as you have described for the knee, but also apply this to the hip. In normal locomotion neither joint in late stance is fully extended as Richard points out. My use of the term “passive stability” was to underline that the external moments are both in extension, thereby removing the need for the extensors to be active at this critical phase of gait. Perhaps the flexors are sufficiently active to control the motion and prevent full/hyper extension rather than the joints “hitting their end stops”. I’ll need to review the emg charts again! This “passive stability” (oops) is only really possible if the thigh is inclined in late stance, and this very often is not the case in eg CP but frequently also in other patholgies I believe. So my argument is that our treatment package should include efforts to try and get the thigh appropriately or at least sufficiently inclined to enable appropriate GRF alignment – oh, and hopefully create an FZ2>BW (as I discovered when I was doing my PhD on the use of AFOs a few decades ago – 1984)…….. I agree with Richard that these joints may be “stable” in other positions eg crouch gait. It’s just that the poor old extensors are having quite a job to achieve this, so it is not “passive” in that sense. Hope the cyclone isn’t too bad this time Chris, and once more it is great to hear from you again. Best wishes, Barry